Volume 18 Number 2
Global Nephrology Nursing Perspectives
Kathy Hill, Suzie Burford and Paul Bennett
For referencing Hill K et al. Global Nephrology Nursing Perspectives. Renal Society of Australasia Journal 2022; 18(2):39-41.
DOI https://doi.org/10.33235/rsaj.18.2.39-41
As we celebrate the 50th year of the Renal Society of Australasia (RSA) it is perhaps timely to discuss the role of the nephrology nurse in Australia and New Zealand and reflect on international comparisons. The prevalence of end stage kidney disease (ESKD) requiring kidney replacement therapy (KRT) has seen a 30% growth since 2010 in Australia and New Zealand (ANZDATA, 2021), with demand for nephrology nurses also increasing in tandem with this increased case load. We know that this is creating workforce pressure in Australia (Hill et al., 2021) and globally (Boyle et al., 2022). We are seeing an increasingly older, frail population which presents multiple challenges in KRT relating to vascular access, home training and clinical stability during treatment (Hill et al., 2021). However, whilst we do have a more complex cohort of patients and some serious workforce challenges, we have also come a long way in nephrology nursing.
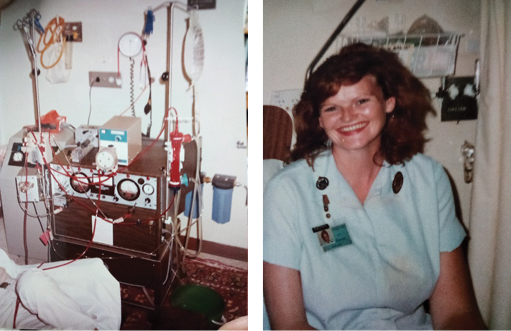
Does anyone recognise the clinical set up in the photo on this page (reproduced courtesy of Berri dialysis unit in South Australia)? If you look closely, you will see carpet on the floor and also a green bucket which, from my recollection, was used to prime out. I started nephrology nursing prior to the introduction of synthetic erythropoietin and regularly administered blood transfusions along with chelating agents to remove the excess iron – thank goodness that is relegated to the past. Have a look at the photo of me in the renal ward of the Royal Darwin Hospital in the 1990s. Today, HD and PD machines have never been safer nor easier to use.
We can also reflect on incredible advances in nephrology and transplant care – you can read about this in more detail in this issue in the discussion on the historical evolution of nephrology by Julian Yaxley and Edward Meagher. It is wonderful to see this submission in tandem with a letter to the Editor from Lynda Moynahan regarding the historical evolution of nephrology nursing education to see how far we have come. As the majority of registered nurses interested in nephrology nursing are introduced to CKD, KRT and kidney supportive care through ‘on the job’ training, the background theory component provided in an accredited course improves critical thinking capabilities, advanced clinical expertise, and leadership for the future nephrology nursing workforce.
Also high on the agenda for nephrology nurses in Australia and New Zealand is the increasing frailty of the renal patient. In this edition of our journal you can read the latest research on frailty by Dr Alice Kennard and colleagues. Another issue high on the nephrology nursing landscape is partnering with consumers for the best research practice and outcomes. One of the main (if not the main) research funders in our region, the NHMRC, have developed a position statement on consumer and community involvement in research (NHMRC, 2016). We can reflect on learnings in relation to the application of this in clinical research practice in the study by author Brett Tarca et al. and learn from the voices of Asian people in NZ in the study conducted by Rachael McLean et al.
What an incredible experience and privilege renal nursing is. For me, it was particularly exciting to be back in Darwin for our annual conference this year. Well done to the RSA and convening team for putting together such a stimulating program – it was great to finally be mingling with colleagues again. Once again, we listened to outstanding keynote speakers and were then able to hear from a large group of nephrology nurses and other renal professionals sharing their research and QA projects, bringing ideas for our own practice and unit protocols. The conference continues to connect our large (and still growing) membership group and we should collectively be very proud to have reached 50 continual years as an organisation.
We hope that you enjoy reading this special edition of the RSAJ.
Kathy Hill
Congratulations to the RSA on this huge milestone of 50 years! My journey in nephrology nursing started approximately 5 years after the birth of RSA, having spent this time in both nephrology nursing practice and nurse education in both Australia and Asia, the latter for the past approximately 20 years.
In Asia, the reported treated incidence and prevalence has increased, especially over the past 10 years (USRDS, 2021); the Asian countries of Taiwan, Japan, South Korea, Thailand, Indonesia and Singapore represent at least 50% of the top countries/regions globally. The increasing epidemiology of CKD and demand for KRT services in Asia is in part due to diabetes prevalence, with Singapore reported to have the highest global percentage (67.5%) of patients with diabetes attributed to ESKD (USRDS, 2021; National Registry of Diseases Office, 2020).
Many Asian countries have nephrology nursing associations/societies that link to the Asian Nephrology Nurses Society which first met in 2009 and has since held meetings every 2 years (ANNS Japan). The country-specific and regional nephrology nursing organisations provide various levels of continuing education and conferences/seminars to support nurses’ development in their specialty nursing role. The increasing demand for service places further stress on healthcare systems in Asia, not least on an increased need for experienced nephrology nurses. Healthcare systems across Asia also utilise various reimbursement models which further contribute to stressors related to access to care, treatment frequency and modes of KRT.
There have been many advances in KRT technologies over the past 50 years that have addressed, primarily, increased safety aspects of therapy delivery and affording increased time for nurses to care, especially relating to the increasing co-morbidity of the CKD patient population – age-related, CVD and diabetes. In Asia this is further confounded by patients seeking less-frequent KRT treatment due to access or healthcare system-reimbursement model costs. Nurses need to be prepared to manage these challenges to ensure patient safety in the short- and long-term and for better patient outcomes.
To further understand the past, present and future of dialysis/nephrology nursing, a short questionnaire was posed to randomly selected nephrology nurses from our region. They reflected that the transition to nephrology/dialysis nursing was a challenge, in particular regarding new knowledge and skills, integrating technology with care, and managing technology. In their current role/practice all responses focused on positively upgrading their knowledge, “making a difference”, improving patients’ outcomes, the “closeness of relationships with patients”, working collaboratively and ensuring continuous learning and acknowledging the “practice setting always changing”. In response to the future of nephrology/dialysis nursing, respondents focussed on nursing leadership in care coordination, increasing the number of nurse practitioners (nurse-led clinics), increasing recognition, more home care, improvement in vascular access care (utilising AI and other technologies), and promoting "electronic data to optimise individualised care delivery".
Staffing (attracting and retaining nurses) and developing the next generation of nephrology nurses will become an imperative to meet current and future challenges. Education programmes need to prepare nurses with a sound foundation in nephrology nursing principles and practice that provides a framework that affords flexibility to adapt knowledge to individualise care delivery. Currently in Singapore we have developed a 200-hour programme for non-renal nurses which has been accredited by the NNA (the Singapore National Nursing Academy, https://www.nna.gov.sg/) and the FME – Singapore Healthcare Professionals (freseniusmedicalcare.sg) which was initiated to address the shortage of specialty dialysis nurses in Singapore. The programme introduces nurses to nephrology nursing, providing a framework grounded in sound principles/knowledge to further advance their specialised nursing competencies. The future looks bright, with opportunities for more recognition and participation in strategic health development for improved outcomes. The major challenge we face is staffing – we need to attract, support and retain the next generation of nephrology/dialysis nurses in order to meet and participate in these opportunities in nursing, nephrology practice and patient care delivery systems – are you ready?
Suzie Burford
The role of the nephrology nurse is highly diverse depending on country income status, health services model, cultural and political status Traditionally, well-resourced regional groups from high income countries – such as the RSA, the European Dialysis and Transplant Nurses Association/European Renal Care Association (EDTNA/ERCA), the Canadian Association of Nephrology Nurses and Technologists (CANNT) and the American Nephrology Nurses Association (ANNA) – have been leaders in the nephrology nursing space. More recently, nephrology nurses have increased their global presence, exemplified by roles in the International Society of Nephrology (ISN), the International Society of Peritoneal Dialysis (ISPD) and the Kidney Disease Improving Global Outcomes (KDIGO) groups.
The ISN Kidney Health Professionals Working Group (ISNKHPWG) is leading the way in understanding global nephrology nursing needs and developing resources and tools relevant for nurses in low and low to middle income countries (LLMICs) (ISN, 2018). To ensure sustainability of regional and local LLMIC support, the ISN is working towards building capacity and supporting nursing education and leadership in LLMICs in Africa, Asia, the Pacific Islands and Latin America by supporting nephrology nurse leaders in these regions (Bennett et al., 2019). Learning needs tools, vascular access and COVID-related resources have been developed with backing from the ISN (Walker & Bennett, 2020).
The ISPD Nursing Liaison Committee (NLC) increasingly contributes to global PD nursing leadership by providing advice and resources offering support to nurses globally with an interest in PD. The ISPD NLC regularly produces replies as a collaborative to “ask the expert questions” posed on the ISPD website. Members of the committee are actively involved in many ISPD initiatives including guideline development and publications (ISPD, 2021).
Nurses are playing an increasing role in KDIGO activity that coordinates global controversies conferences, guideline development, commentaries, reports and other resources that contribute to improving the care and outcomes of patients with kidney disease (KDIGO, 2021b). Nephrology nurses were highly active in the recent 2021 Controversies Conference on Home Dialysis where a critical, in-depth review of factors that either positively or negatively impacted home dialysis utilisation and approaches and strategies that expand the use of home dialysis was reviewed (KDIGO, 2021a). A greater number of nurses contributed to the KDIGO Controversies Conference on Symptom-Based Complications in Dialysis which aimed to identify optimal means for diagnosing, managing and treating symptom-based complications in patients undergoing dialysis therapy considering patient-centred issues, perspectives, values, preferences and quality of life (KDIGO, 2022).
A/Prof Paul Bennett
Author(s)
Dr Kathy Hill PhD MPH GradCert (Neph) BN RN
Editor in Chief, RSAJ
Suzie Burford FMC Asia
Fresenius Medical Care Asia
A/Prof Paul Bennett
University of South Australia
Correspondence to Dr Kathy Hill, Lecturer in Nursing, School of Nursing and Midwifery City East Campus,
University of South Australia, SA, Australia
Email Kathy.Hill@unisa.edu.au
References
Australia and New Zealand Dialysis and Transplant Registry (ANZDATA). (2021). 44th annual report. Retrieved from https://www.anzdata.org.au/report/anzdata-44th-annual-report-2021-data-to-2020/
Bennett, P. N., Walker, R. C., Trask, M., Claus, S., Luyckx, V., Castille, C., Ashuntantang, G., & Richards, M. (2019). The International Society of Nephrology Nurse Working Group: Engaging nephrology nurses globally. Kidney International Reports, 4, 3–7.
Boyle, S., Washington, R., McCann, P., Koul, S., McLarney, B., & Gadegbeku, C. A. (2022). The nephrology nursing shortage: Insights from a pandemic. American Journal of Kidney Disease, 79, 113–116.
Hill, K., Neylon, K., Gunn, K., Jesudason, S., Sharplin, G., Britton, A., Donnelly, F., Atkins, I., & Eckert, M. (2021). Sustaining the renal nursing workforce. Renal Society of Australasia Journal, 17, 39–45.
International Society of Nephrology (ISN). (2018). About ISN. Retrieved from https://www.theisn.org/about-isn/supporting-groups/other-topics-and-initiatives-supporting-groups/#khpwg
International Society of Peritoneal Dialysis (ISPD). (2021). Increasing the voice of nurses in our society. Retrieved from https://ispd.org/increasing-the-voice-of-nurses-in-our-society/
Kidney Disease Improving Global Outcomes (KDIGO). (2021a). Controversies conference on home dialysis. Retrieved from https://kdigo.org/conferences/hd/
Kidney Disease Improving Global Outcomes (KDIGO). (2021b). KDIGO: What we do. Retrieved from https://kdigo.org/mission/
Kidney Disease Improving Global Outcomes (KDIGO). (2022). Controversies conference on symptom-based complications in dialysis. Retrieved from https://kdigo.org/conferences/symptom-based-complications-in-dialysis/
National Registry of Diseases Office. (2020). Singapore Renal Registry annual report 2020. Retrieved from https://www.nrdo.gov.sg/docs/librariesprovider3/default-document-library/srr-annual-report-2020.pdf?sfvrsn=658dd717_0
NHMRC. (2016). Statement on consumer and community involvement in health and medical research. Retrieved from https://www.nhmrc.gov.au/sites/default/files/documents/reports/consumer-community-involvement.pdf
Walker, R. C., & Bennett, P. N. (2020). The International Society of Nephrology and the Renal Society of Australasia: Towards a global impact. Renal Society of Australasia Journal, 16, 6–7.
USRDS. (2021). Annual report 2021. Chapter 11: International comparisons. Retrieved from https://adr.usrds.org/2021/end-stage-renal-disease/11-international-comparisons
